If I Knew Then What I Know Now
Understanding my Endo Journey
I’ve been having more conversations lately—the kind that start quietly, almost hesitantly, and then spill open. Conversations with women who have found themselves in eerily similar situations, whispering stories they once thought were too embarrassing, too “gross,” too “un-lady-like” to say out loud. And what I’m realizing is this: our vulnerability is our strength.
The very things we’ve been taught to hide are often the things that connect us most. When we speak them—plainly, honestly—we normalize them. We create space. We make it easier for someone else to exhale and think, oh… it’s not just me. So this is me, leaning all the way in.
And in that spirit—of saying the quiet things out loud, of choosing honesty over comfort—I’m going to take you back to a moment I didn’t have the language for at the time. One that felt isolating, confusing, and, if I’m being honest… a little humiliating.
It was the morning after my best friend’s wedding and I was in crippling pain. For 5 hours I went between standing in a scalding shower, from sitting on the toilet, to fetal position on the hotel bathroom floor. All the while Sean is sitting on the bed attempting to provide support when all I could do was cry and yell for him to come in— only for me to scream “leave me alone” seconds later.
Reluctantly I let him reach out to a fellow bridesmaid, and empathetic friend who deals with a chronic disease of her own to see if she had any laxatives. She watched as I chased 4 pills with a cup of coffee praying to god the pain would subside. At this point we only had about 45 minutes to check out of our hotel, drop our car off to the rental car company, and check into the airport for our cross-country flight. [We couldn’t fly the next day because Sean was starting his new position Monday.] So I sucked it up. I put on a pair of spandex shorts lined with period pads, and braced for impact. It was the longest flight I had ever had to endure.
One week later I found myself in the same position —except this time, it was in Sean’s parents’ downstairs bathroom. Sean and I traveled to the Peninsula to walk in an SVS (Society for Vascular Surgery) event, “Walk for Vascular Health”, spend time with his parents, meet Sean’s new colleagues and raise awareness. On our travels over I started to feel crampy —a scary feeling familiar to the week prior. I brushed it off thinking it was just my stomach announcing its hunger until I had to excuse myself from their kitchen to use the bathroom. I was mortified. Aside from feeling like a disappointing girlfriend who couldn’t show up for her guy, I also couldn’t help but wonder what his parents thought as they left for the event. Hours later Sean and I departed, sitz bath in hand, and headed for an unforgettable start to our lives in California.
The next day I was in the ER talking to a Colorectal Dr and getting a CT scan. He was certain I was dealing with Colitis but was also worried I may have contracted a disease from our recent travels in Thailand. What were my results? Full. Of. Shit.
In fact, I had a hard stool stuck in my rectum the size of a small baby. When I asked “Why did this happen?”, they couldn’t give me a clear answer. As I laid in the hospital bed waiting for the Dr to complete a digital rectal exam [stick his finger up my ass hole], I locked eyes with Sean as we nervously laughed about the current situation. It was at that moment I knew I chose my perfect match. After completing a saline enema, they sent me on my way with prescribed laxatives and told me to avoid spicy foods and start incorporating Miralax into my daily routine. Yay!
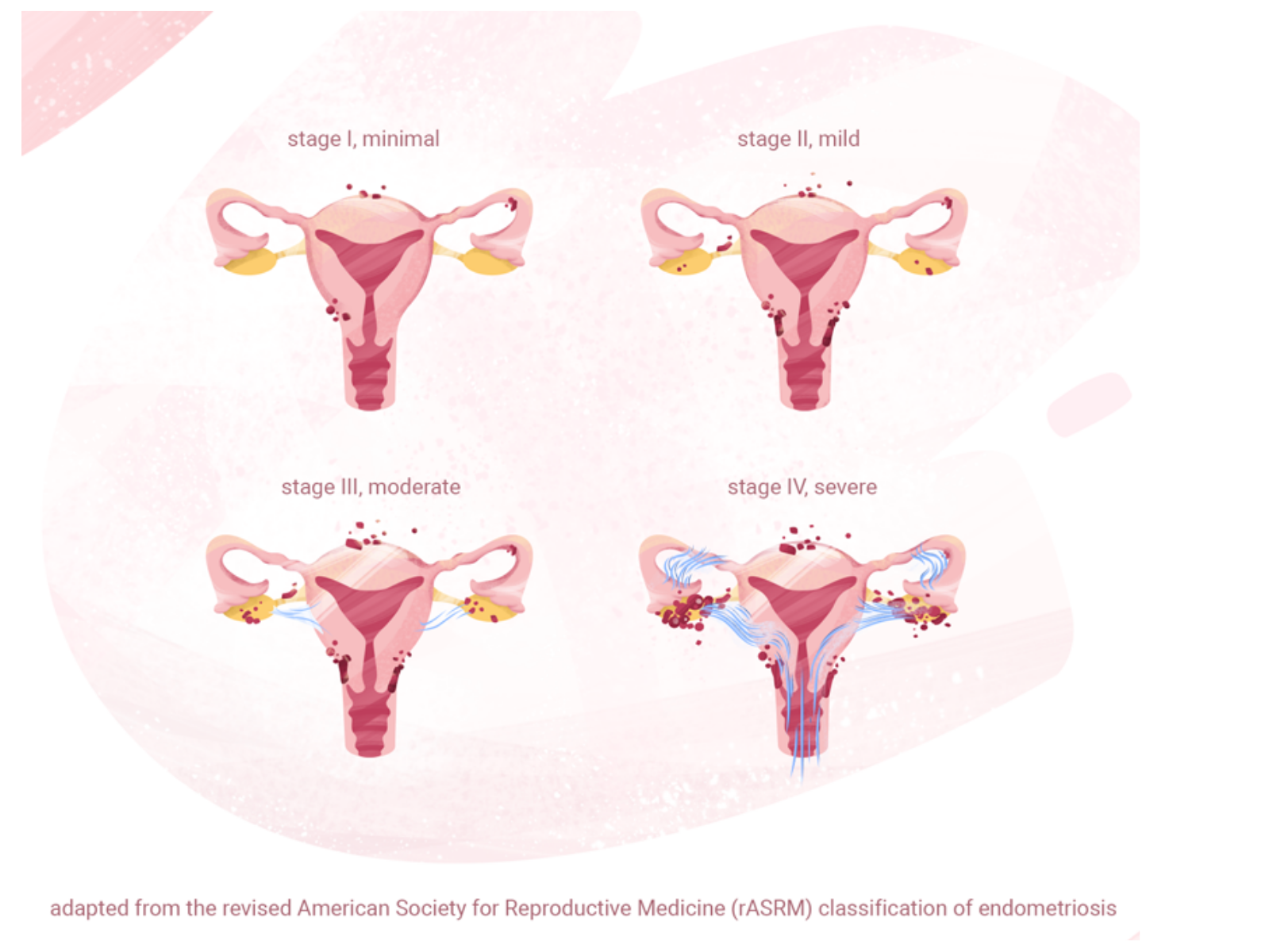
Fast forward to months later. I am staring at Dr. Nezhat’s transvaginal ultrasound screen as he explains my endometriosis has spread to my cervix, ovaries, bladder AND intestine. He explained that most of the endometrial tissue is attached to my sigmoid colon and would explain why I am experiencing severe constipation and painful defecation due to its invasive and inflammatory nature.
I had no idea that Endometriosis could infiltrate other organs. I always assumed it was just about menstruation because that’s what I have always been told. But Endometriosis is a whole body disease— endometrial lesions have been found on every major organ in the body.
If there’s one thing I’ve learned through all of this, it’s that silence doesn’t serve us—connection does. The more we share, the more we begin to see just how many of us are navigating this quietly, behind closed doors. So let’s keep talking about it—the uncomfortable, the messy, the misunderstood. Because awareness matters. Advocacy matters. Funding matters. And research is crucial. Not just for me, but for every woman still searching for answers, relief, and validation.
Follow my full Endo Journey on Instagram, Facebook, TikTok and Pinterest (@calicottagecutie).
What is Endometriosis?
Endometriosis is a whole-body (systemic) chronic inflammatory disease that can cause incapacitating pain, organ failure, infertility, and other severe medical consequences if not adequately treated by an experienced specialist.
Although symptoms can vary considerably, the most common are:
extremely painful periods, pain just before or after your period, pelvic pain at any time during the month, pain during or after sexual intercourse, difficulty getting pregnant (infertility), nausea and vomiting, severe abdominal bloating, pain during ovulation, pain or bleeding with bowel movements, other bowel symptoms (ie, pain with bowel movements/ constipation/ diarrhea intestinal pain/upset stomach), other bowel/gastrointestinal symptoms (acid reflux, loss of appetite, nausea with eating), pain or bleeding with urination, other bladder symptoms (difficulty voiding/urgency/frequent urination/ incontinence), pain in the lower back, pain in the groin area, heavy periods, more frequent periods, other, irregular bleeding, fainting/falling unconscious (due to pain), pain that mimics appendicitis, pain that mimics celiac disease, pain that mimics Crohn’s Disease and/or irritable bowel syndrome, pain that mimics interstitial cystitis, fatigue
Endometriosis Resources
Dr. Camran Nezhat, MD, FACOG, FACS
Dr Camran Nezhat is internationally recognized as the best and most experienced endometriosis excision surgeon in the world. He has performed more than 20,000 Video assisted laparoscopic and robotic assisted surgeries for endometriosis—to our knowledge more than any living surgeon. Patients from around the globe seek his expertise, as his meticulous excision techniques have set the highest standard of care in endometriosis surgery.
Widely known as the “Father of Modern Operative Laparoscopy and modern day surgery ,” Dr. Nezhat pioneered video-assisted laparoscopic and endoscopic surgery even for complex conditions, including bowel, bladder, diaphragm, and liver resections for endometriosis. His groundbreaking minimally invasive surgical techniques revolutionized surgery, profoundly improving surgical outcomes. This opened new pathways for surgeons in gynecology, reproductive endocrinology and infertility, urology, colorectal surgery, thoracic surgery, and beyond to help their patients.
The EndoMarch Global Movement leads the fight for urgently-needed improvement to the way we diagnose and treat endometriosis, a potentially crippling, whole-body chronic disease, affecting an estimated 200 million people around the world. The movement has ignited an international response from women and men in 60+ countries and counting, leading to dramatically increased awareness and policy changes around the world, including a bipartisan bill to increase federal funding for endometriosis research and public awareness campaigns.
Endometriosis Foundation of America
The Endometriosis Foundation of America (EndoFound) strives to increase disease recognition, provide advocacy, facilitate expert surgical training, and fund landmark endometriosis research.
Their mission is to elevate the discourse around endometriosis beyond medicine, into the realm of equality and human rights. By championing early diagnosis, advancing expert surgical training, and integrating endometriosis education into medical schools and universities, we ensure that the next generation of physicians — and society at large — recognize women’s pain as valid, urgent, and deserving of answers. Education is extended not only to women but also to men, families, and communities, reshaping how reproductive health is understood and respected.